AI-driven Mental Health Decision Support Enhances Clinician Resilience and Preparedness

Key Takeaways

Limbic Access improves clinician wellbeing by reducing anxiety, stress, and uncertainty

Limbic Access improves clinician performance during assessments and effectively reduces cognitive load

AI-powered decision support tools may help reduce burnout risk and its effects on service quality and patient outcomes


Background
Mental health services are facing unprecedented demand, placing significant pressure on clinicians to conduct timely and effective patient assessments. Rising staff turnover and burnout threatens service quality across many countries. This study examined whether providing clinical information collected via Limbic Access, an AI-enabled decision support tool for mental health assessments, could improve clinician wellbeing and performance during patient assessments.
Methods
We surveyed mental health clinicians from nine mental health services on how the information provided by an AI-enabled decision-support tool impacted their experience with conducting clinical assessments. Clinicians reported on assessments where information from the AI tool was available, as well as when it was not (e.g., primary care physician referrals or telephone intakes). Outcomes included clinician wellbeing, task performance, and cognitive load during assessments, with additional analyses assessing the influence of moderating factors, such as clinician experience, workload, and exposure to the tool.
Results
Relative to traditional methods, assessments supported by information provided by the AI tool were associated with significantly higher clinician wellbeing and task performance, and significantly lower cognitive load, irrespective of the clinician’s experience. These benefits were magnified by workload.
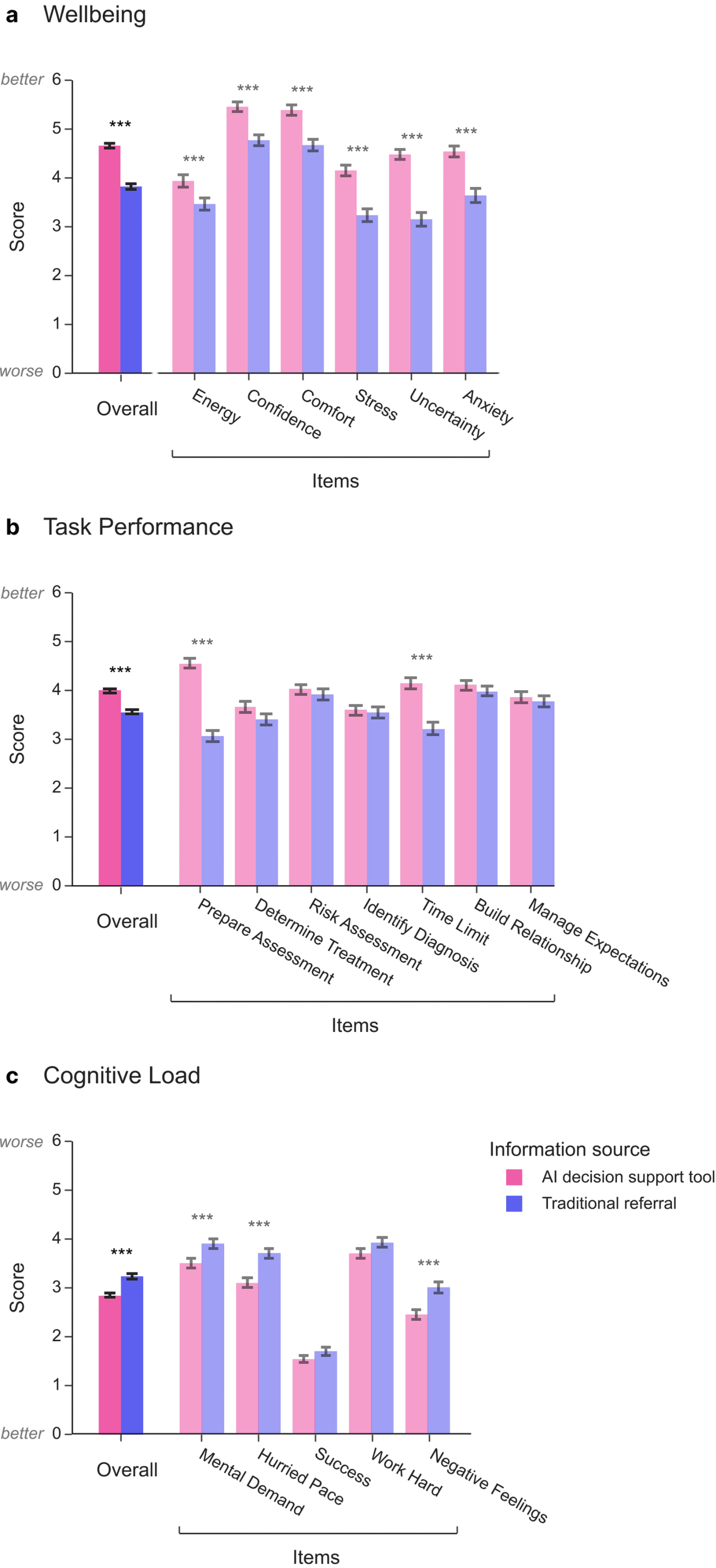
Limbic Access was associated with a statistically significant improvement in clinician wellbeing, reporting more energy, confidence and comfort, and less stress, uncertainty and anxiety during assessments
Limbic Access led to a statistically significant reduction in cognitive load, resulting in less mental demand compared to standard processes
Limbic Access was associated with a clinically significant improvement in clinician performance during initial assessments, with clinicians reporting feeling more prepared and better able to complete assessments within the appointment time
Conclusions
These findings provide evidence that AI-powered pre-assessment tools can enhance clinician experience by improving wellbeing, boosting task performance, and reducing cognitive burden. By addressing systemic drivers of burnout, such tools offer a scalable intervention to support workforce sustainability and service quality in mental health care.

